defence against disease
Our bodies provide an excellent environment for many microbes which can make us ill once they are inside us. We are warm and have a ready supply of nutrients available. However, we are also very well adapted to stop most microbes getting in. If those pesky pathogens do happen to sneak their way into our bodies, we have a number of mechanisms to deal with them, and we are very good at naturally defending ourselves against infection. We will study all of these elements as well as looking at how medical and scientific developments have helped us to cope with infectious diseases.
|
So, what is a pathogen?
A microorganism that can cause infectious disease. You become ill when large numbers of these microbes enter your body. The main pathogens that we are concerned about are bacteria and viruses Bacteria - Reproduce rapidly in our bodies and produce toxins (poisons) that make us feel ill. Remember that although bacteria are all around us, on us and in us, NOT ALL BACTERIA ARE BAD. Illnesses caused by bacteria include cholera, food poisoning and tuberculosis BBC BITESIZE contains fantastic revision pages on how the body defends itself against disease along with some nice animations. There's even a quiz so you can check your progress. Another lovely site here!
|
Viruses - Much smaller than bacteria (indeed, some viruses can infect bacteria). Unlike bacteria, ALL viruses are bad, although they aren't all bad for us. Viruses cannot reproduce outside of a cell so once inside our body, they invade a cell, rapidly reproduce and then burst out of that cell, spreading viruses in the process. It is the damage that they do to our cells that makes us feel ill.
Illnesses caused by by viruses include AIDS, chickenpox and flu Ever wondered why you get a fever when you're ill? Find out here
If you're bored of reading, try this interactive revision guide
|
Important scientists throughout history
|
Using his ingeniously simple swan-neck flask experiment, Pasteur disproved the theory of Spontaneous Generation once and for all, and went on to show that microbes not only cause food to go off, but also that they cause some infectious diseases. The technique of pasteurisation (using heat to kill microbes) is still used today and is named after this fabulous Frenchman
Ways to prevent the spread of infection in hospital:
|
This bald boffin revolutionised hygiene standards in hospitals in the mid-19th century. He observed that women whose babies were delivered by doctors were much more likely to die than those who were attended by midwives. He noticed that the doctors were going straight from the dissecting dead bodies to the delivery ward without washing their hands - yuck! Presumably they were carrying some kind of infectious agent? He insisted that the doctors washed their hands before delivering babies. Immediately the death rate fell.
|
This Essex-boy started the use of antiseptic chemicals to destroy pathogens before they caused infection in operating theatres. He found that if you sprayed the patient’s wound with carbolic
acid, it didn’t go septic and gangrene didn’t set in. Prior to this ~50% of patients who had ops died. Lister also experimented with hand-washing and sterilising instruments. Lister's work was partially inspired by the great Pasteur - a wonderful example of the importance of scientific publication
|
|
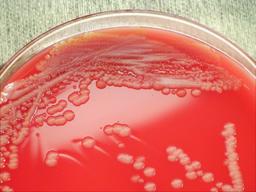
Growing uncontaminated cultures of bacteria
You can grow cultures in flasks or on agar plates. Here are my TOP TIPS for making sure that your culture is not contaminated. All tips apply to plate and liquid culture:
|
Ways to destroy pathogens: Heating - to 120 °C under pressure in an autoclave. Great for metal and glass but plastic will melt Radioactivity - gamma radiation is often used to sterilise plastics Disinfectants - chemicals that kill pathogens. Only used on non-living surfaces as would damage our cells Antiseptics - chemicals that kill pathogens on living tissues. Weaker than disinfectants |
HOW WHITE BLOOD CELLS (WBC) PROTECT YOU FROM DISEASE
White blood cells defend out internal environment from pathogens. They form part of our immune system. But how do they do it?
White blood cells defend out internal environment from pathogens. They form part of our immune system. But how do they do it?
|
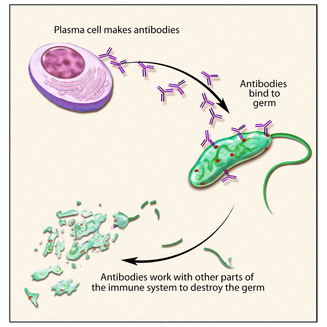
PRODUCING ANTIBODIES
Every cell expresses unique proteins on their coats called antigens. The antigens on microbes that enter your body aren't recognised by your immune system (which is constantly surveying) as they are different from your own ones. Special WBCs called lymphocytes produce proteins called antibodies which are specific for these antigens. These antibodies target the pathogens by binding to the antigens on their coat. This causes the pathogens to clump together resulting in them either being neutralised (ie, they are incapacitated and so die off) or ingested by the phagocytes. Antibodies act against both viruses and bacteria. These antibodies make use immune to infection by the same pathogen again. |
iNGESTING MICROBES
Also known as phagocytosis. Some WBCs (known as phagocytes) ingest pathogens. Enzymes within the phagocyte digest the pathogen, thereby destroying it. This is a very general, non-specific defence mechanism. Check out this real-life footage of a phagocyte crawling after a bacterium PRODUCING ANTITOXINS
These neutralise the toxins (poisons) produced by pathogens, principally by bacteria Other ways your body has of defending itself against the invasion of microbes:
|

It's all about the letter A Antigen - protein expressed on the coat of the pathogen. This is what the antibody recognises Antibody - protein produced by the WBC to target the antigen on the pathogen and destroy it (bacteria and viruses) Antibiotic - drug designed to cure bacterial diseases by killing the bacteria (NOT viruses) inside your body Antiseptic - liquid which kills microbes in the environment |

V is for vaccination
Vaccination (or immunisation as it's also known) is defined as the injection of dead or weakened (live) pathogens into our body which results in the production of antibodies by the WBCs. It was developed by Edward Jenner (see the Geek of the Week archive for more info). Scientists are able to exploit the natural defence mechanisms of the immune system in order to develop vaccines which will provide us with immunity against a wide range of pathogens. As you know, we have special WBCs called 'memory cells'. These cells act like guard dogs, continuously monitoring the blood for invaders. As their name suggests, the memory cells 'remember' the antibody that is specific for any given pathogen that we have been exposed to before. Of course, they don't actually 'remember' (they don't have brains!). What memory cells do is that they recognise the antigens on the coat of the pathogen and QUICKLY produce the appropriate antibodies for that antigen. This means that we don't have to have every antibody that we have ever produced rushing around our body all of the time. It also means that if we are exposed to a pathogen that we have been vaccinated against, our body will respond and kill it off without us even knowing about it - genius! |
STRETCCCCCCCCCCCHHHHHHHHHH YOURSELF!
- Can you think of any diseases that don't have vaccines?
- Why might that be?
- Why might pharmaceutical (drug) companies choose not to develop certain vaccines?
- Do you think there might be any dangers or consequences of totally eradicating an infectious disease?
Look here for more information and immunity and vaccination

Antibiotics
Penicillin, the founder member of this group of drugs, was first discovered in the 1920s by Alexander Fleming (for more information, see Geek of the Week!). Unlike painkillers such as paracetamol and ibuprofen which simply relieve the symptoms of your illness, antibiotics act on the cause. These medicines work inside your body to kill the disease-causing bacteria. Remember, antibiotics do not act on viruses. Antibiotics act to kill bacteria by either disrupting one of the processes that they need to survive, or by preventing them reproducing. 
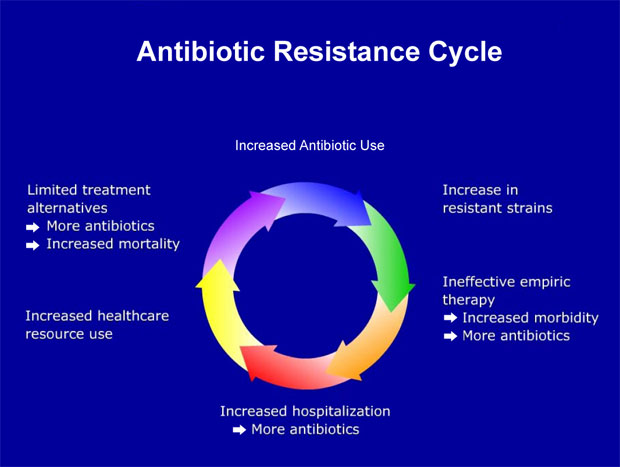
Due to the emergence of new strains of antibiotic-resistant bacteria, it is important for new antibiotics to be developed. However, this takes a long time. Currently there is a serious concern worldwide about the emergence of new strains of bacteria that are effectively untreatable. Imagine what that would be like. We could go back to a healthcare system like it would have been prior to the work of Fleming, Florey and Chain.
|
Changing pathogens
Mutations (changes in their genetic material) of pathogens produces new strains MRSA is an example of a mutant bacterial strain, and SARS is an example of a mutant viral strain. The flu virus also regularly mutates. When bacteria mutate they often become resistant to antibiotics. Indeed, MRSA stands for 'methicillin-resistant Staphylococcus aureus'. Staphylococcus aureus is a form of bacteria that usually lives quite happily on our skin and in our nose. However, as a result of natural selection, a certain strain of Staphylococcus aureus mutated to become resistant to methicillin (an antibiotic) and is thus called MRSA There are several ways in which we can help to prevent the development of more antibiotic-resistant forms of bacteria
|
Remember: if a strain of bacteria becomes antibiotic resistant, it doesn't mean that they are resistant to all antibiotics. Some bacteria will only be resistant to one antibiotic. The Superbugs are generally resistant to many different types of antibiotic.
Also, it is important to remember that the mutant strains of bacteria are no more infectious that the unmutated form. They are simply more difficult to treat.
Also, it is important to remember that the mutant strains of bacteria are no more infectious that the unmutated form. They are simply more difficult to treat.
|
Look at this fantastic resource to examine the relevant of the emergence of antibiotic-resistant bacteria in today's society. This issue is also the focus of the Longitude Prize 2014.
|